What is a preventer inhaler?
A preventer inhaler is the main way to treat asthma. It contains a low dose of steroid medicine to keep down inflammation and swelling in your airways.
Giving the medicine through an inhaler means it can get to your airways more easily.
“The steroids in your preventer inhaler are called corticosteroids,” says Dr Andy Whittamore, Asthma + Lung UK’s in-house GP. “They are a copy of the steroids our bodies produce naturally. They are not the same as steroids used by bodybuilders.”
Your preventer inhaler is not for asthma attacks
You need to use your reliever inhaler when symptoms come on. Your reliever inhaler acts quickly when you have an asthma attack, so keep it with you at all times.
Types of preventer inhaler
There are different types of corticosteroid preventer inhaler. They can be different colours, but most are brown.
- Metered dose inhalers (MDIs) give the medicine in a spray form (aerosol). This is the one you can use with a spacer.
- Breath actuated inhalers (BAIs) release a spray of medicine when you begin to inhale.
- Dry powder inhalers (DPIs) give the medicine in a dry powder instead of a spray.
You can talk to your GP or asthma nurse about the best inhaler device for you.
If you find your inhaler difficult to use, you can see if there is another device you might find easier.
What are the benefits of preventer inhalers?
Your preventer inhaler stops swelling and inflammation building up in your airways. This means you’re less likely to react badly to your asthma triggers.
If you take your preventer inhaler every day, you should notice:
- you’re less sensitive to your asthma triggers
- you don’t need your reliever inhaler as much
- you can do more during the day
- you’re sleeping better at night
- it’s easier to do exercise
When do I take it?
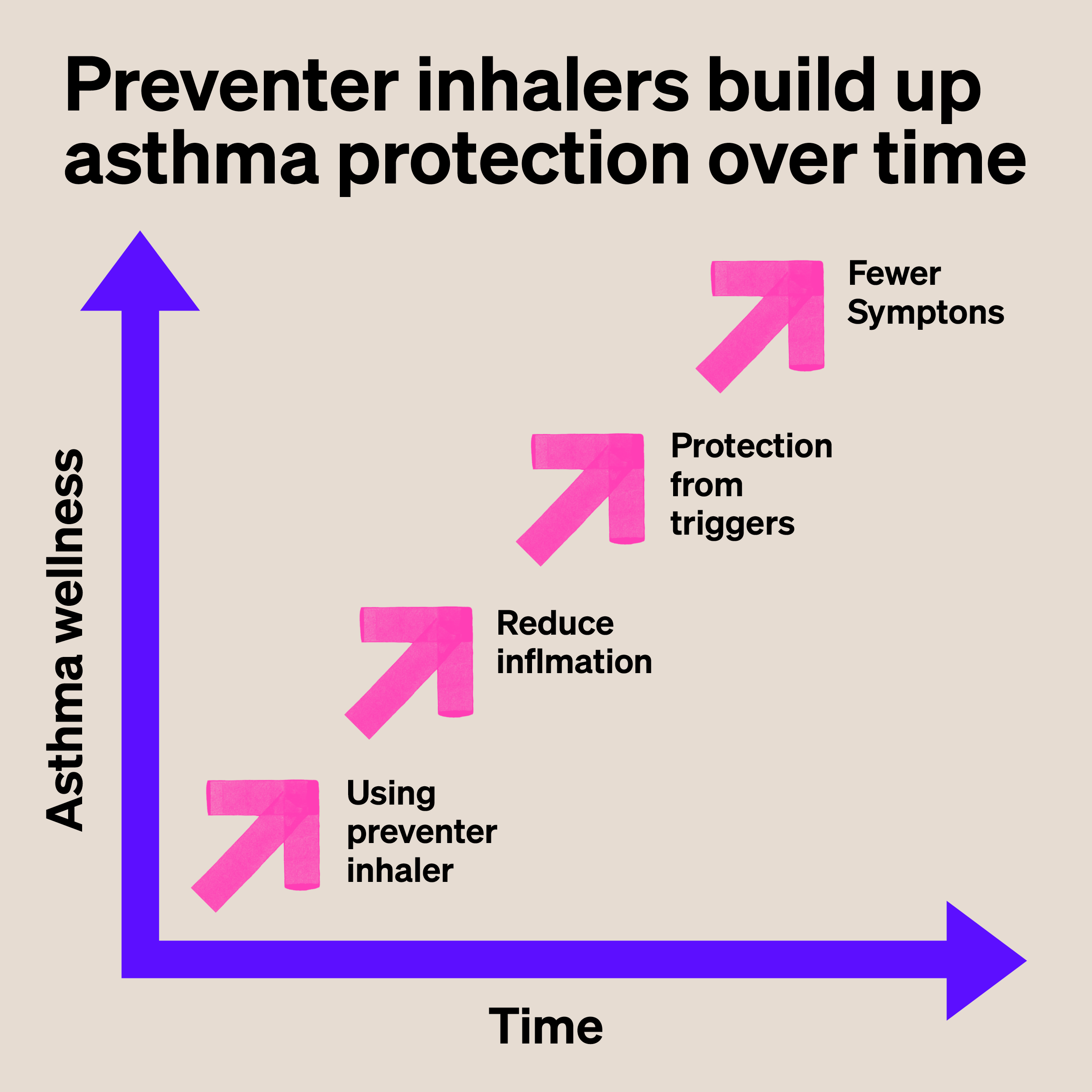
You need to take your preventer inhaler every day, as prescribed, even if you think your asthma is okay. This is so it can build up protection in your airways over time.
Most people need to take their preventer inhaler twice a day, once in the morning and once in the evening.
Your GP or asthma nurse will tell you when you need to take yours and how many puffs to take. They can write this down in your asthma action plan.
How do I know I’m taking it properly?
Whatever inhaler you're prescribed you need to know how to use it in the best way. This is known as good inhaler technique. A good inhaler technique helps get the medicine to the lungs where it’s needed.
- Ask your GP or asthma nurse to show you how to use your inhaler.
- Ask your pharmacist to check your inhaler technique.
- Watch our inhaler videos.
- Use a spacer with your metered dose inhaler (MDI). This is so you don't have to worry about getting the timing right for pressing the inhaler and breathing in.
Are there any side effects?
Preventer inhalers are the safest and best way for most people to lower their risk of asthma symptoms and attacks.
As with all medicines, there are possible side effects. But the risk of side effects from taking a low dose of inhaled preventer medicine is very small. The risk of not taking your preventer inhaler and having asthma symptoms or an asthma attack is higher.
Common side effects include:
- a sore throat
- a hoarse voice
- a mouth infection called thrush
The good news is these can often be completely avoided. A good inhaler technique means the medicine doesn’t stay in your mouth and throat but gets down into your airways where it’s needed.
- Find out the best way to take your inhaler. All inhalers have a different technique.
- Use a spacer if you’ve got an MDI inhaler.
- Rinse your mouth and spit out after using your inhaler.
- Go to regular asthma reviews to check you’re on the right dose
“Your GP or asthma nurse will always aim to keep you on the lowest dose possible to keep you well,” says Dr Andy. “The low dose of steroid medicine in your preventer inhaler means you’re less likely to need higher doses of rescue steroids for an asthma attack.”
Find out more about possible side effects if you’re taking higher doses of steroids for your asthma.
Do I need a steroid card for a steroid preventer inhaler?
Your GP should give you a steroid emergency card if you’re on a high dose preventer inhaler.
A steroid card lets doctors and other healthcare professionals know you take steroids at a high dose.
This is important in emergency situations, as your body may not produce enough natural steroids to help you deal with illness or injury. In this situation, doctors will need to give you extra corticosteroids.
Make sure you always carry your steroid card with you.
Do not stop steroids suddenly
If you’ve been prescribed steroids, whether as tablets, liquid or in an inhaler, make sure you take them every day as prescribed. Do not stop taking your steroid medication suddenly unless you have been told to by your GP or asthma nurse.
Preventer inhaler top tips
Get into a good routine
Keep your preventer inhaler somewhere that reminds you to take it for example, next to something else you do every day. Or try a reminder app on your phone. Sticking to a good routine makes taking your inhaler an everyday habit like brushing your teeth.
Don’t run out of preventer medicine
Make sure you contact your GP for a new prescription before your preventer inhaler runs out. Some inhaler devices have a counter to show how many doses are left. When the numbers on the counter turn red, it’s time to contact your GP for a new prescription.
You can arrange repeat prescriptions with your local pharmacy to make things easier.
Take old inhalers back to the pharmacy
You can return your used inhalers to any pharmacy. This means they can be disposed of in a safe and environmentally friendly way.
If you have concerns about the environmental impact of inhalers, it’s good to know that alongside considering the best device for you and your asthma, your GP can also look at the carbon footprint of different inhalers.
Inhaler choices
Did you know that managing your lung condition well could help you feel your best and help the environment? We’ve partnered with the NHS to support you to make changes, so that you can live better with your lung condition and help the environment at the same time.
Find out more about inhaler choices.

Get support
Call our Helpline for support with your condition. Get advice on your medicines, symptoms or travelling with a lung condition, or just call us to say hello.




